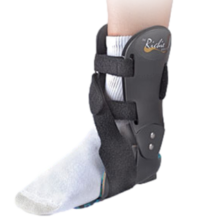
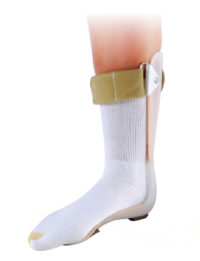
PREFERRED BRACING OPTION
The Richie Brace® family of AFOs has been successfully implemented for thousands of patients over 25 years; treating the most challenging foot & ankle pathologies. The lightweight, low-profile design makes it the preferred option over traditional AFOs.
PREFERRED BRACING OPTION
The Richie Brace® family of AFOs has been successfully implemented for thousands of patients over 25 years; treating the most challenging foot & ankle pathologies. The lightweight, low-profile design makes it the preferred option over traditional AFOs.
TREATMENT GUIDE BY INDICATION
Key Points of Biomechanical Control
- Prevent internal rotation of the tibia which limits subluxation of the talonavicular joint
- Prevent abduction of the forefoot
- Preserve ankle joint motion when possible
Brace Recommendations
- Stage 1: Use foot orthoses initially, and consider the Richie Brace® Standard if treatment fails
- Stage 2: Flexible hindfoot: Richie Brace® Standard
- Stage 3: Rigid hindfoot: Richie Brace® Restricted Hinge with Medial Arch Suspender
Casting
For Richie Brace® Standard or Richie Brace® Restricted Hinge with Arch Suspender, plaster splints or the STS Ankle Casting Sock may be used.
NOTE: Medial and lateral malleoli markings are required.
Modifications
- 6mm medial heel skive
- Lateral flange
- For heavier patients: 4.0 poly shell material
- For enhanced stiffness: flat rearfoot post replaces standard stabilizer bar and crepe arch filler
- For severe forefoot abduction: add forefoot strap
- Stage 4 deformity: severe valgus ankle with DJD of ankle and subtalar joints:
- Richie Brace® Gauntlet or Richie Brace® California AFO
- Cast with STS midleg sock, capture height (minimum) of 7 inches
Removing Forefoot Supinatus
For all patients with adult-acquired flatfoot:
- Patient must be casted nonweight-bearing, neutral suspension technique
- Be sure to push down on 1st ray and remove all forefoot supinatus (this is most important when treating PTTD)
PERONEAL TIBIAL TENDINOPATHY
Treatment Goal
Limit ankle inversion and plantarflexion
Brace Recommendation
Richie Brace® Restricted Hinge
It is important to measure any tibial varum in relaxed stance and to have the lab adjust limb uprights for any tibial varum exceeding 10°
Brace Modifications
- Lateral heel skive
- Posting: valgus RF post | 2° – 4 °
- Extended forefoot valgus sulcus wedge | 2° – 4 °
ANTERIOR TIBIAL TENDINOPATHY
Treatment Goal
Limit ankle plantarflexion
Brace Recommendation
Richie Brace® Dynamic Assist
NOTE: Consider the OTC Dynamic Assist if there is minimal foot deformity
When to choose the Richie Brace® Dynamic Assist
The Richie Brace® Dynamic Assist will achieve a heel strike and a normal gait pattern for patients with dropfoot if the following patient conditions are present:
- Range of motion in the ankle joint is able to reach 90° (foot to leg)
- Posterior calf musculature is strong
- Good knee stability
- Lack of hindfoot deformity NOTE: Stroke patients, as well as patients with common peroneal nerve injuries, meet this criteria.
When to choose the Richie Brace® Solid AFO
The Richie Brace® Dynamic Assist is preferred for all dropfoot conditions, but will fail if the following patient conditions are present:
- Knee instability
- Fixed equinus
- Spasticity
- Weak calf (consider Solid AFO or Restricted Hinge)
In these cases, the most appropriate brace is the Richie Brace® Solid AFO.
When to choose the Richie Brace® Restricted Hinge
The Richie Brace® Dynamic Assist is preferred for all dropfoot conditions, but will fail if the following patient conditions are present:
- Severe varus
- Severe valgus
- Weak calf (consider Richie Brace® Solid AFO or Richie Brace® Restricted Hinge)
In these cases, the most appropriate Richie Brace® is the Restricted Hinge.
Additionally, these points are important to consider with choosing the Richie Brace® Restricted Hinge:
Dropfoot with Severe Varus or Valgus Deformity
In Charcot-Marie-Tooth Disease or other common peroneal nerve injuries, there is often an acquired cavo-adducto-varus deformity of the foot.
The varus condition combined with dropfoot requires the following prescription modifications:
- Measure tibial varum and ask the lab to bend uprights when tibial varum exceeds 10°
- Add 6mm lateral heel skive
- Add 4° valgus sulcus wedge (extended forefoot post)
- Add 4° valgus rearfoot post for extreme cases
Severe varus conditions that arise from neuromuscular pathologies often require footwear modifications such as a valgus midsole wedge.
Dropfoot with Equinus
When equinus is present, this condition is better controlled with the Richie Brace® Restricted Hinge. The brace must hold the foot in the maximum dorsiflexion position that is allowed to each specific patient. This requires that the footplate be aligned at the ankle in a plantarflexed position. This position must be measured and designated by the prescribing doctor based upon measurements of maximum range of ankle dorsiflexion available to that patient. This requires the laboratory to make some modifications based upon the deformity captured in the impression cast. However, the STS mid-leg casting sock must be used!
Additionally, this allows accurate measurement of fixed equinus but requires the practitioner to:
- Cast the patient in a non-weight bearing position with the knee flexed to at least 45°.
- Dorsiflex the ankle to end range during the casting process.
- When this brace is fixed in equinus, a heel lift should be applied to bring the limb uprights to perpendicular. The heel lift will also aid in achieving a heel strike when equinus deformity is present.
- Remember to apply a heel lift to the contralateral shoe!
When to choose the Richie Brace® Standard
The Richie Brace® Standard (with flat rearfoot post) is recommended for patients with subtalar arthritis.
- If the patient also has significant varus or valgus alignment of the calcaneus, add medial heel skive (valgus deformity) or lateral heel skive (varus deformity) to decompress the affected side of the subtalar joint
When to choose the Richie Brace® Restricted Hinge
- The Richie Brace® Restricted Hinge is recommended for patients with ankle arthritis.
Patient Evaluation Note:
Check for fixed equinus and adjust the angle of footplate accordingly. If the ankle mortise is compressed in varus/valgus direction, add a medial heel skive to decompress valgus deformity or add a lateral heel skive to decompress a varus deformity. Posting of the brace in rearfoot, forefoot, or both can also be utilized to decompress frontal plane deformity of the ankle.
When to choose the Richie Brace® Gauntlet or the Richie Brace® California AFO
- The Richie Brace® Gauntlet or the Richie Brace® California AFO are recommended when there is global DJD of the ankle, subtalar joint, and midfoot and where there is severe deformity
NOTE: In most cases, the Richie Brace® Restricted Hinge will work just as well and offers far better shoe fit and ease of wearing.
The Richie Brace® Standard is ideally suited to treat chronic ankle instability.
Key Biomechanical Features:
- Unrestricted pure sagittal plan ankle motion
- Restriction of frontal plan inversion and transverse plan external rotation
- Contoured total contact footplate for maximal proprioceptive input
Key Points of Patient Evaluation
Hindfoot Varus
- If there is NO significant varus alignment of the hindfoot, no need for any additional modifications
- If there IS significant varus alignment of the hindfoot, the following modifications are recommended:
- 6mm lateral heel skive
- 2–4 degree valgus sulcus wedge
- Medial flange
Brace Recommendations
Brace Recommendations
Richie AeroSpring Plantar Fascia Offloading System
We recommend the Richie AeroSpring Plantar Fascia Offloading System when patients are showing little to no positive response to traditional treatment options.
Mechanism
During standing and walking, the plantar fascia is subjected to elongation strain by:
- Achilles tendon located immediately proximal
- “Tie rod” component of the truss mechanism of the arch
- Tension created by the windlass mechanism at the first metatarsophalangeal joint
With severe recalcitrant cases of chronic plantar heel pain, clinicians often prescribe walking boots which address some, but not all, of these damaging mechanisms. Walking boots have numerous disadvantages which lead to poor patient compliance:
- Limb length discrepancy causing hip and back pain
- Bulky and heavy causing knee pain
- Need for removal when driving an automobile
The Richie AeroSpring Bracing System® has been developed to simultaneously address all three of three loading mechanisms of the plantar fascia. The result is a three-prong approach to minimize the mechanical strain on the plantar fascia during standing and walking. Superior to walking boots, the Richie AeroSpring Plantar Fascia Offloading System addresses the biomechanics of foot function to reduce strain on the plantar fascia. A custom balanced orthotic footbed contours to the medial and lateral longitudinal arches. Heel wedges combined with the shank contour of the foot orthoses have been documented to offload the central band of the plantar fascia. The patented Richie ArchLock™ offloads the medial-central band of the plantar fascia. Compared to walking boots, this dynamic brace system does not create a limb length discrepancy and can easily be disengaged for driving an automobile.
CLINICAL INDICATIONS BY AFO
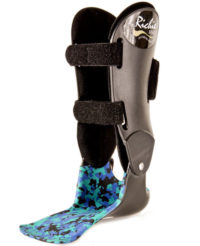
- PTTD (mild-to-moderate)
- Lateral Ankle Instability
- Peroneal tendinopathy
- Cavo-varus deformity
STS Casting Sock Size: Ankle
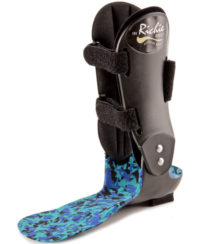
- PTTD (moderate-to-severe w/ subluxed TN Joint)
- Dropfoot (equinus Severe varus/valgus; weak calf)
- DJD (ankle or rearfoot w/ dropfoot & spasticity)
- Peroneal Tendinopathy (order with lateral arch suspender)
- Lateral Ankle Instability (severe; order with lateral arch suspender)
- Peroneal Nerve Injury (fixed varus in hindfoot/ankle; order with lateral arch suspender)
STS Casting Sock Size: Ankle
STS Casting Sock Size: Mid-Leg
STS Casting Sock Size: Mid-Leg
CLINICAL INDICATIONS BY OTC BRACE
- Acute ankle sprain
- Tendinopathy of the foot or ankle
- Interim brace before custom AFO
STS Casting Sock Size: NA
See product details for sizing chart

- Dropfoot secondary to CVA or nerve injury
- Mild muscular dystrophy
- Diabetic neuropathy
- Charcot-Marie-Tooth Disease
- Interim brace before custom AFO
STS Casting Sock Size: NA
See product details for sizing chart